Priya Garg,
DTMH 2015
There is a small, smiling two-year old girl, sitting upright on a sunflower yellow blanket. A metal bed-rest props her up, one hand outstretched, fingers splayed joyfully towards the camera, a huge grin lights up her face, her right leg completely covered in white wrapped bandaging, urinary catheter discretely in situ.
She sits in the middle of a paediatric ward in Sudan. Alone. Her parents had brought her to hospital, and, devastatingly, due to her disability, never came back to pick her up.
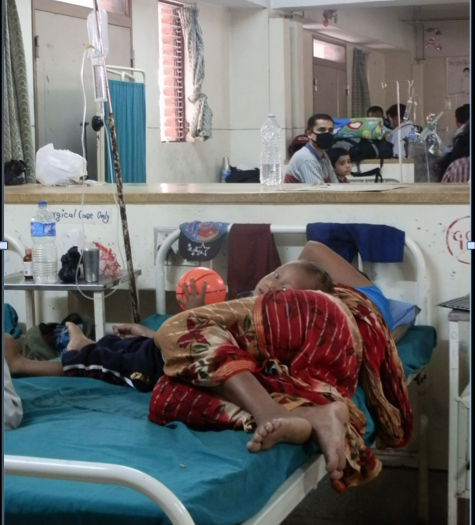
Where does she go? Who looks after her?
With minimal available social care, what will happen to her now?
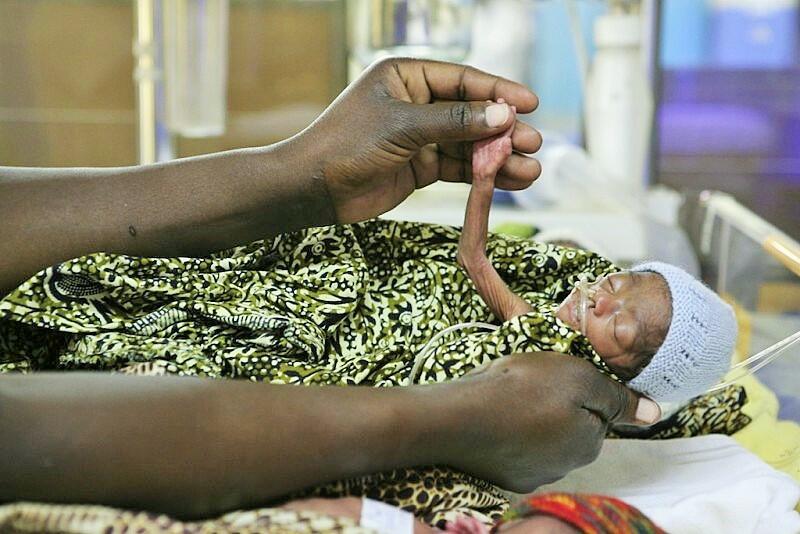
Discussing ‘Neonatal Care in the Tropics’, ex-paediatrician now public health physician, Dr Sylvia Garry, tells us of her brutal, heartbreaking experiences in many low income settings. These include the abandonment of children with multiple congenital abnormalities and bleak, desperate requests from families for the euthanasia of their babies with severe medical conditions.
This was due to a number of factors such as lack of social support, limited education, cultural conflict, the stigma of disease or having just too many mouths to feed with no perceived ability to care for another child with new, extra needs. As silence fell across the lecture hall, we all imagined ourselves in this staggeringly complex situation. ‘What would you do?’ Dr Garry asked us.
In this scenario, where and how does one draw the line between clinician and, simply, person, patient and child?
‘UNICEF’ data from 2003 suggested that 110 newborn babies in Khartoum were abandoned every month, with 50% estimated to die before receiving any assistance.
A photograph of another tiny boy flashed across the screen, brown eyes large, a silver metal cross looped on multi-coloured beads laced over his neck. Delicate plastic nasal cannulae link to his nostrils, providing the vital oxygen needed for a chronic, irrecoverable post-infective lung condition. Without it, he would not be able to survive. His sister, hair scraped back into a bun, nestles her head lovingly on to his shoulder.
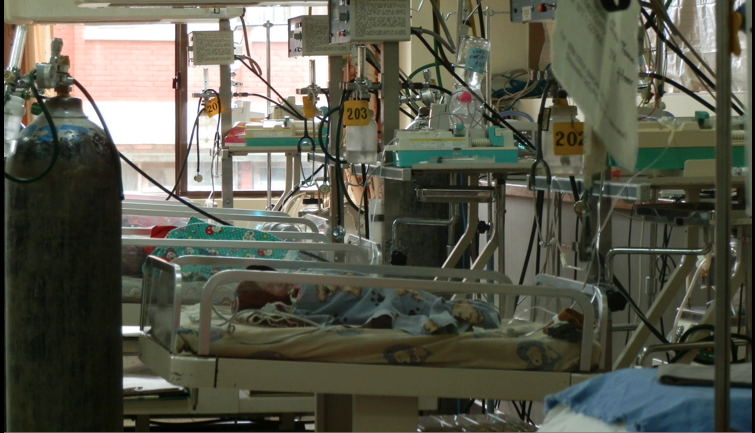
What now, if another child appears? An acutely unwell child, rushed through the department, wheezing, perhaps coughing, desaturating and requiring emergency oxygen to prevent their death? What if this new baby had a potentially reversible condition? Yet, to give oxygen to this child, to save their life, what if, due to lack of supplies, this meant removing the cylinder from the first little boy? What if this meant taking treatment from one, to save another?
Through personally experienced cases, Dr Garry reminded us of not only the reality and stark, sometimes gut-wrenching challenges of working in a low resource setting, but also gave us invaluable pieces of advice. This included focusing on knowing your professional and emotional limits, of working within the ethical framework of autonomy, beneficence, non-maleficence and justice to help decision-making when faced with incredibly difficult scenarios.
Hence, in the wake of complex ethics, alongside consultant Dr Jim Pauling, we also learnt a few basics of paediatrics. These include key facts we could implement in the field in order to address some of the issues we may encounter, one of which was the theory of ‘Kangaroo Mother Care’, now a staple guideline of the ‘WHO.’ This is a simple design focusing on skin-to-skin contact, breastfeeding and bonding, and aimed to be adaptable to local conditions. As well as promoting better neonatal care, fundamentally, ‘Kangaroo Mother Care’ is thought to reduce the rates of infant neglect and abandonment by positively encouraging maternal attachment.
Inspiringly, here we could see, how a straightforward, low-cost intervention, could dramatically change the lives of many children and parents across the world. We also saw how practically, we as students and doctors, could learn the skills, to help, encourage and carry out that change in seemingly overwhelming situations.