Intervention Packages
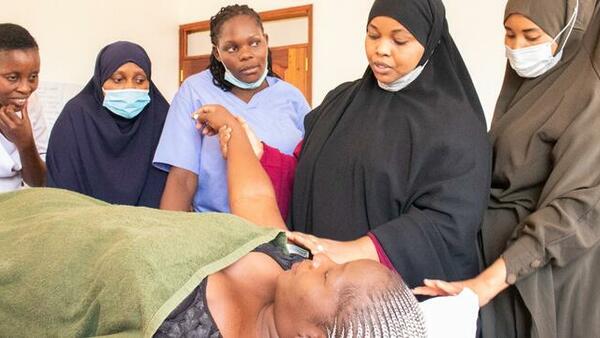
ANC&PNC workshop package
Developed in 2017 by LSTM in collaboration with more than fifty maternal and newborn health experts across ten low and middle-income countries, the competency-based workshop package for healthcare providers working in low and middle-income countries addresses the identified health needs of mothers and babies during and after pregnancy with integration of care across three main diseases – HIV/AIDS, TB and malaria. The workshop covers physical, mental and social aspects of maternal and newborn health. The focus is on evidence-based screening, therapeutic interventions and health promotion during and after pregnancy. It also supports health workers in providing respectful maternity care and in screening for and managing domestic violence and depression during and after pregnancy.

Quality Improvement
To support Quality Improvement, the Takeda/Global Fund programme in 5 countries (Chad, Kenya, Nigeria, Tanzania and Togo) focuses on standards-based (clinical) audit1, which is the systematic review of the quality of care compared to standards of care agreed by all the relevant health managers and providers.
The Quality Improvement interventions utilise materials developed by LSTM, including published manuals for improving the quality of Antenatal (ANC) and Postnatal (PNC) care.
To make the course accessible to as many health providers as possible and to be cost-effective, the existing QI course was modified to use a blended learning approach.

Advanced Obstetric and Anaesthetic Skills
Following the successful implementation and evaluation of the LSTM-Emergency Obstetric and Newborn Care training package and our work around Maternal Death Surveillance and Response, this training offers additional support to improve the availability and quality of care at comprehensive emergency obstetric care facilities.
Basic Emergency Obstetric Care Package
There are pre-designed materials for delivery of the training package that include a simple manual and a Facilitators Guide. In addition, a generic set of obstetric and newborn mannequins that have been extensively field-tested, is used to facilitate this training.
Maternal Death Surveillance and Response
The EmOC & QoC unit is represented on the WHO Maternal, Perinatal Death Surveillance and Response Technical Working Group, and the WHO Technical Advisory Group on Maternal Mortality and Maternal Cause of Death Estimation. The unit is also developing, piloting, and evaluating midwifery education modules in Maternal and Perinatal Death Surveillance with support from UNFPA midwifery branch.
The EmOC & QoC unit has designed and piloted a Global MDSR Accountability framework, it is expected that if this framework is adopted, it will create a pathway achieving the ‘Response’ in MDSR and drive accountability for maternal health at all levels of the health system.
Mentoring training package
We use evidence-based learning and teaching methods suitable for adult learning and which have been shown to result in improved communication, and improved evidence-based practice. Our 2-3-day training course delivers teaching and interactive discussions (80% practical/simulation/hands-on, 20% short lectures) regarding the mentorship process and techniques for good mentorship together with scenarios to practice mentorship encounters with the aim of developing mentorship competencies for clinical mentors. To ensure sustainability and continuity we support Ministry of Health to adapt existing mentoring package based on this evidence-based approach. The training is complemented by a manual, that contains various tools.
Pre-Service Workstream
Liverpool School of Tropical Medicine promotes and supports sustainable strategies to reduce maternal and perinatal mortality and morbidity in Kenya.
This is through investments and research aimed at strengthening the capacity(link is external)(opens in a new tab) of pre-service training institutions and midwifery and reproductive health educators and trainers.
Additionally, we conduct implementation research on improving the quality of pre-service midwifery education and training through a bundle of interventions.