
International Day of the Midwife 2023
Together again: from evidence to reality
Globally there are more than four births every second, and on International Day of the Midwife, we are celebrating the caregivers that have improved health outcomes for mothers and babies across the world.

Health professionals with a midwifery specialism at LSTM have been instrumental in helping to improve the quality of health care and services to women across the globe.
Maternal, neonatal and paediatric conditions continue to pose major global health risks, especially in lower- and middle-income settings. Complications around pregnancy and childbirth; infections such as with malaria, HIV and tuberculosis during pregnancy and severe acute malnutrition and undernutrition amongst children under the age of 5 still pose significant challenges despite progress made over the past years.
Professor Dame Tina Lavander is head of LSTM’s Centre for Childbirth, Women’s and Newborn Health, working with the Lugina Africa Midwives Research Network, she leads the NIHR Global Health Research Group on Stillbirth Prevention and Management in Sub-Saharan Africa. The Group is a unique midwife-led research partnership addressing the critical lack of research around stillbirth and identify best practice to support families in Kenya, Malawi, Uganda, Tanzania, Zambia and Zimbabwe.
Women and families affected by stillbirth need appropriate and respectful care, but misconceptions and shame associated with bereavement often results in isolation and limited support from communities and their needs are often not met by the healthcare system.
Professor Dame Tina said: “The research team had a shared vision to change the lives of women, babies, and families. We have successfully delivered a programme of research with direct benefits for practice, while giving midwives their voice and the skills and confidence to make a real difference to women and their babies in the future.”
Reducing deaths through the training of midwives
We know that globally nurses and midwives are the leading health providers during childbirth globally, so the quality of their education is absolutely vital for the survival of mothers and their babies.
In Kenya, LSTM is undertaking a UK funded programme by the Foreign Commonwealth and Development Office (FCDO) on improving maternal and newborn health and quality midwifery education.

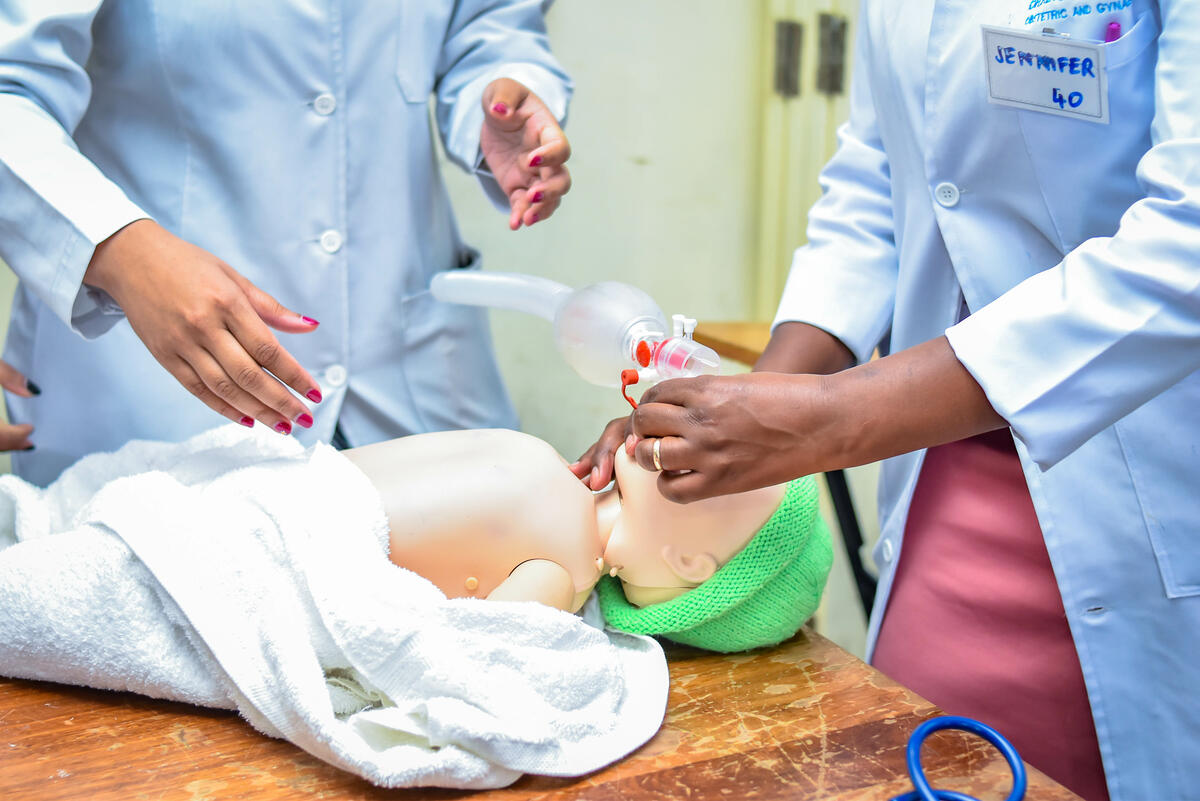
In total, 129 training institutions in Kenya are appropriately trained to teach Emergency Obstetric and Newborn Care (EmONC) within the updated curriculum, equipping health care workers with the skills, competencies and confidents to conduct competent deliveries and care has reduced maternal and newborn mortality.
The Emergency Obstetric Care and Quality of Care Unit at LSTM commissioned a short mini-series of podcasts focussing on sharing lessons learned from the programme Improving Quality of Maternal and Newborn health. One of the episodes, looked at improving the quality of midwifery education in Kenya.
A programme designed to improve the quality of maternal and newborn babies in Kenya is now reaping the rewards regionally, nationally, and internationally. As a result, other countries including Cambodia and Nigeria are set to benefit from best practice knowledge in midwifery.
Professor Charles Ameh, Head of LSTM’s Department of International Public Health, said: “Now we have supported the facility based on reviews of maternal deaths so that we can learn from each maternal death - so the systems in Kenya are strengthened in terms of providing that next generation of healthcare. Furthermore, when we look at the medical schools - the postgraduate schools - and their capacity to improve the quality of their research.
“The FCDO funded programme has been implemented by the Emergency Obstetric Care and Quality of Care Unit. We started by setting up a confidential enquiry into maternal deaths so a robust, objective way of understanding of why women had died. We set up a system in Kenya which was only the second country in Africa, at the time, that had such a system. As part of it, we developed this and piloted it in several settings which included Cambodia, Nigeria and in Kenya, working closely with the investors in Kenya and now this has gone on to impact how both medical students and residents are trained.”
Engagement and partnership can lead to better outcomes for mothers
Good engagement and partnership across communities is crucial in order to improve the quality of care when mothers are giving birth.
A string of improvements have been implemented across 47 counties in Kenya, relating to mothers giving birth, with the aim of further reducing the number of deaths in mothers and babies through learning experiences.
Lucy Nyaga, is a Medical Anthropologist and Country Director for LSTM Kenya. She said: “The maternal, perinatal death, surveillance and response normally referred to as MPDSR, normally involves systematic analysis of trends in deaths.
“This is important because it can identify health systems barriers and inspire local solutions to prevent such deaths in the future and this is really a role of the government. Having good engagement and partnership is key. This is not a one man or a one institution show. You have to engage a number of stakeholders from across the government, from across implementing partners from professional bodies.
“They all have their role in ensuring that the quality of care provided to mothers and their babies, while pregnant, is really engaged. I would say partnership in ensuring successful maternal and perinatal death is key.”
In total LSTM has trained more than 54,000 students across Kenya, helping to ensure midwifery services are consistent and of high quality in different areas. The programme has enabled the curriculum in nursing, clinical medicine in relation to integrating emergency obstetrics, and newborn care.
There have been 40 campuses across Kenya that have been equipped with emergency obstetrics and newborn care equipment. This has made it possible for quality training to take place and has been instrumental in ensuring 233 nursing, midwifery and clinical medicine lecturers being trained.
Best practice can then be shared across the world, so more lives are saved. If you would like to learn more through our podcasts, please click here.
Studying maternal and child health at LSTM
At LSTM, we also have a range of post graduate courses on offer – one relates to Tropical Paediatrics. Blending clinical and research skills, students will learn from experts in global child health. Discovery and discussion will lead to an independent research project focussing on improving care, treatment, or service delivery in maternal and child health.


