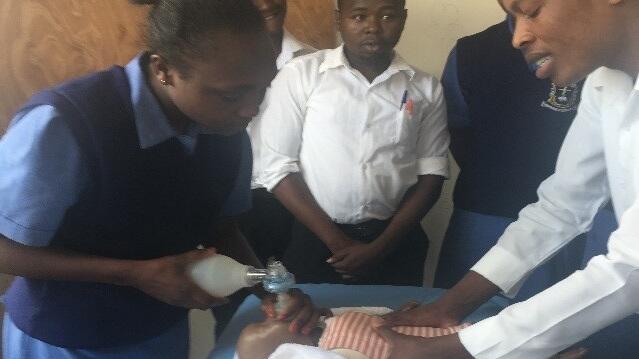
Background
Kenya is not on track to meeting the SDG targets of less than 70/100,000 (currently at 342/100,000) maternal mortality ratio and 12/1000 (currently at 22/1000) newborn mortality rate by 2030. To achieve this, a functioning health system that includes “skilled health personnel” (SHP), previously known as skilled birth attendants, who are competent to provide care during labour and childbirth is essential.

However, the largely didactic pre-service clinical officers and midwifery training curriculum, inadequate and inequitable distribution of SHP, insufficient education capacity to supply the desired levels of health workers needed by the market in the country are challenges to achieving quality maternity care and universal health coverage. The Constitution of Kenya and Kenya Health Policy 2014 – 2030 shifts the focus to achieve universal health coverage by improving the production of health workers (numbers and quality) by aligning curricula and training with needs and competencies, promoting multi-skilling and multitasking and enhancing the skills, knowledge and attitudes of the health workforce required to deliver health goals; and ensuring the appropriate and equitable distribution of health workers in facilities.
Definition of skilled health personnel
World Health Organization (WHO), International Confederation of Midwives (ICM) and International Federation of Gynecology and Obstetrics (FIGO) define skilled health personnel as competent maternal and newborn health (MNH) professional educated, trained and regulated to national and international standards and competent to identify and manage or refer women and/or newborns with complications thus can perform all signal functions of emergency maternal and newborn care (EmONC) to optimize the health and wellbeing of women and newborns.
Emergency obstetrics care (EmOC)

An estimated 15 per cent of pregnant women will develop a complication during pregnancy, childbirth or the puerperium, which will require EmOC. Emergency obstetric care is defined as the collective minimum set of medical interventions (or bundle of care) required to prevent or manage the main obstetric complications (haemorrhage, preeclampsia or eclampsia, sepsis, complications of obstructed labour or abortion) and newborn complications (birth asphyxia).
The critical role of midwifery services
Midwifery services are cost-effective and could avert 83% of all maternal deaths, stillbirths and neonatal deaths. In Kenya, midwifery and obstetrics workforce plays a leading role in health service delivery, providing assistance during birth in 58% of all births (KDHS 2014).
The WHO 2006 report on ‘Working Together for Health’ ranks Kenya among the 57 HRH-crisis countries characterized by shortages and lack of skilled and equitably distributed healthcare workers. The country has an average of 21 doctors and 100 nurses per 100,000 population compared to the WHO recommended minimum staffing level of 36 doctors and 356 nurses, respectively. Training and deployment of mid-level health care workers has been used to address skilled health workers shortages in low- and middle-income countries including Kenya. As at November 2018, Kenya had 19,085 clinical officers registered by the Clinical Officers Council, (compared to 76,000 nurses/midwives and 11,000 doctors) (source: KHSSP July 2018 – June 2023), making them the second-highest available SHP workforce in the country.
Clinical Officers in Kenya
Recent research has shown that non-physician clinicians (NPCs), maybe a viable solution to bringing physician-type services closer to people that need them. In Kenya, NPCs are currently known as Clinical Officers (COs) and are regulated by the Clinical Officers Council, an institution mandated under the Clinical Officers Act (CAP 260) established in 1988 to oversee their training, registration and licensing. They are trained to address Kenyans’ health needs and deliver high quality clinical and surgical health services. General clinical officers are trained for three years in clinical medicine and surgery, and additional training of 12 months (in either Paediatrics; Lung and skin diseases; Mental Health and Psychiatry; or Orthopaedics and Trauma) or 18 months (in either Reproductive Health; Anaesthesia; Ear, Nose and Throat (ENT) and Audiology; Ophthalmology Advanced Refraction and Low Vision; or Ophthalmology and cataract surgery) is needed to be a Specialist Clinical Officer. A clinical officer's scope of practise depends on one's training and experience, jurisdiction and workplace policies.In Malawi, for instance, a clinical officer performs all routine surgical and obstetric operations such as exploratory laparotomy, emergency orthopaedics and caesarean section. However, in Kenya, Tanzania and Mozambique one has to undergo further specialized training to perform such caesarean sections and emergency orthopaedics safely.

Pre-service clinical medicine training in Kenya
While the training of clinical officers started in 1928 with hospital-based certificate programs, today clinical officers are trained at diploma and degree levels in 47 institutions across Kenya. The first university in Kenya to train clinical officers was Egerton University in 1999. Kenya has three core curricula for the training of clinical officers: 4-year Bachelor of Science, Clinical Medicine and Community Health; 3-year Diploma in Clinical Medicine and 1.5-year Higher National Diploma in Reproductive Health that aim to spearhead the attainment of high healthcare standards in the country, in line with Vision 2030. The introduction of the newly developed Higher National Diploma in Reproductive Health for Clinical Officers in 2015 was a major milestone in the provision of comprehensive reproductive health services. These officers work to contribute to the provision of quality service and reduce maternal, neonatal and child mortality through programmes like Beyond Zero Campaign.
Core training curricula review
The Ministry of Health, through the Clinical Officers Council, regulates the COs training and practice and reviews and approves the core curricula of the universities and colleges. As the only professional regulatory body for all cadres of COs in Kenya, it accredits training institutions and programmes of study for the clinical medicine professions and prescribes the training syllabi (commonly referred to as core curricula) used to develop the curricula for training at training institutions. It reviews core training curricula every 5 years, and the last review was in 2015. The updated definition of skilled health personnel and the requisite competencies in the provision of essential care needed for women and newborns creates an opportunity to update the clinical medicine – reproductive health training core curricula. This is timely to accelerate the drive towards the ambitious SDGs.
Pre-service clinical medicine – reproductive health training like other types of medical training has been criticized for lacking in the skills competency aspects for its graduates who require further exposure through internships and clinical attachments to acquire the necessary clinical skills. It is doubtful that clinical officer graduates from the three training levels have the requisite competencies needed to function adequately as SHP in health facilities without direct supervision of an experienced midwife, clinical officer or medical doctor with EmONC skills.
Updated pre-service core curricula
A review and update of the clinical medicine – reproductive health training guidelines to reflect internationally recognized standard competencies by integrating the competency-based EmOC training at the pre-service level in MNH is essential. Liverpool School of Tropical Medicine – Centre for Maternal and Newborn Health provided both financial and technical support to COC in updating the clinical medicine – reproductive health training core curricula to reflect the current SHP competencies integrating the EmOC and maternal and perinatal death surveillance and response (MPDSR) – key in achieving quality of care. The emergency obstetrics care skills competencies included are effective clinical communication using the Situation Background Assessment & Recommendation (SBAR) tool, use of partograph in labour, birthing procedures, assisted vaginal birth through vacuum extraction, management of obstetric emergencies – shoulder dystocia, manual removal of retained placenta, caesarean section and active management of postpartum haemorrhage, use of the modified early obstetrics warning score (MEOWS) chart for critical maternity patients among others. Clinical officer lecturers will be upskilled through training and mentoring based on the delivery of the competency-based updated curricula. This investment in midwifery and obstetrics workforce training has the potential to accelerate the achievement of SDG 3 for Kenya.