Authors
Irene Nyaoke, Senior Technical Officer - Liverpool School of Tropical Medicine (LSTM) Kenya
Martin Eyinda, Technical Officer – Liverpool School of Tropical Medicine (LSTM) Kenya
Onesmus Muchemi, Technical Officer – Liverpool School of Tropical Medicine (LSTM) Kenya
Lucy Nyaga, Country Director- Liverpool School of Tropical Medicine (LSTM) Kenya
Rael Mutai, Regional Technical Advisor- Liverpool School of Tropical Medicine (LSTM) Kenya
Hellen Siria –Reproductive Health Coordinator, Uasin Gishu County, (Kenya)
Charles Ameh, Professor Global Health, Head Emergency Obstetric and Quality of Care Unit, Liverpool School of Tropical Medicine (LSTM) United Kingdom.
While the world has committed to reduce global Maternal Mortality Ratio (MMR) to less than 70 per 100,000 live births (SDG target 3.1) by 2030, in Kenya, MMR stands at 355 deaths per 100,000 live births (KNBS, 2019). Kenya has registered increased coverage of ANC, SBA and PNC services and yet MMR has more or less stagnated (362/100,000 in 2014) over the past decade. This is a major concern for Kenya and reflects the quality of care provided at the health facilities. The first CEMD report 2017 identified sub-standard care in 9 out of 10 maternal deaths in Kenya. Based on the obstetric transition model described by Souza et al, quality of care improvements are required to reduce MMR below 300/100, 000 live births.
Achieving coverage targets of the Ending Preventable Maternal Mortality (EPMM) and Every Newborn Action Plan (ENAP) indicators such as Antenatal care (at least 4 ANC contacts), skilled attendants at birth (SBA) and timely postnatal care (within the first 2 days after birth) remain critical in reducing maternal and perinatal morbidity and mortality (WHO 2023 report). However, research is needed to develop and test indicators for tracking change in quality of care.
Quality improvement (QI) in health care is a systematic process of assessing performance of a health system and its services, identifying gaps and causes, and introducing measures to improve quality and monitoring the impact. In June 2022, the Kenya Ministry of Health, (MoH) launched and disseminated technical guidelines on MNH standards for improving quality of care in health facilities. These, however, are not yet widely utilised and monitored at the facility level. Additionally, through Department of Health Standards, Quality Assurance and Regulation, the Kenya Quality Model for Health (KQMH) framework was issued by MOH. This is designed to guide regular assessment, improvement and maintenance of delivery of quality health services at all levels of the health care in Kenya. The framework works through Quality Improvement teams (QIT).
Liverpool School of Tropical Medicine (LSTM) in collaboration with National MoH and county health departments of Uasin Gishu, Vihiga and Garissa is implementing a three-year (2021 – 2023) program, Quality improvement for Integrated HIV, TB, and Malaria services during Antenatal and Postnatal Care in Kenya. The program (funded by Takeda CSR program through Global Fund) supports 61 health facilities and has, to-date trained almost 300 frontline health care providers and 46 trainers in integrated ANC and PNC; and quality improvement (QI) standards for ANC and PNC. Using the national MNH standards, 97% (n = 59) of the targeted health facilities are currently implementing standards-based audits (StBA) to reorganise patient care with the aim of ensuring that mothers and babies receive high quality care and subsequently achieve better health outcomes.
Ben Too, is a nurse at Ngenyilel Health centre since 2013 undertook Quality Improvement training by LSTM in January 2023. After the training, he returned to the health facility and shared with the Facility Manager (Janet) about what he had learned.
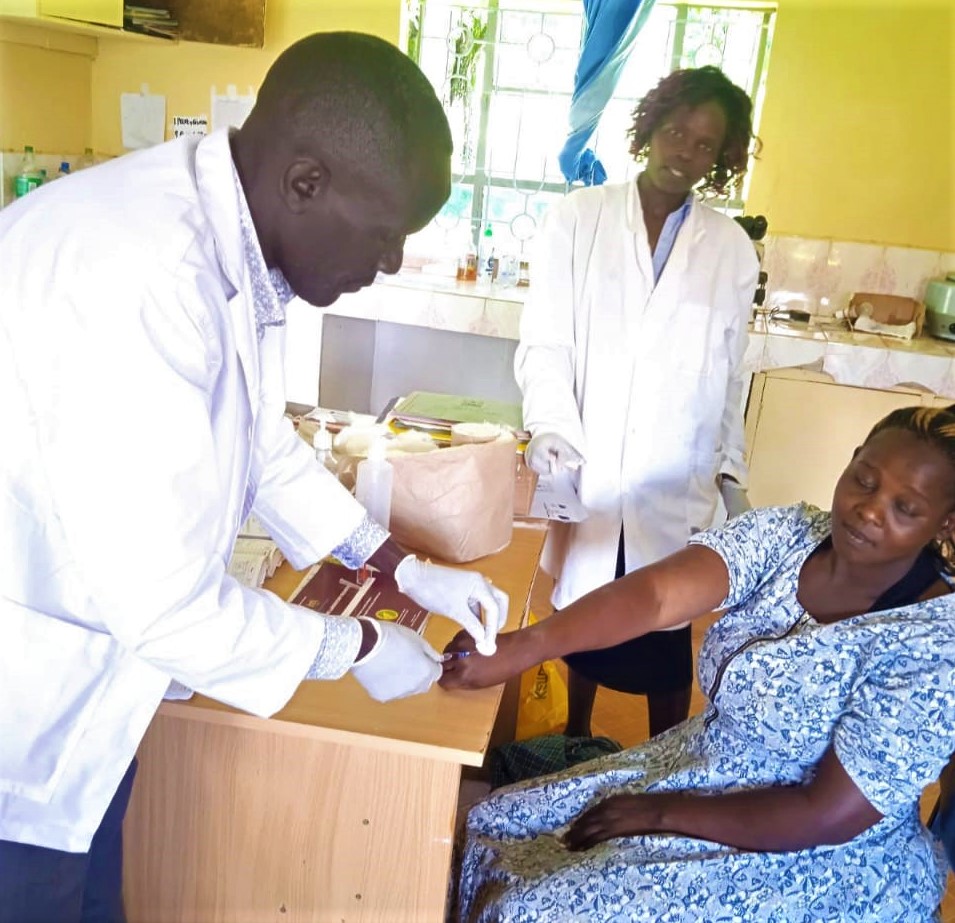
As a result of Ben’s participation in the training, a Quality Improvement Team (QIT) for Ngenyilel Health centre was constituted primarily to coordinate and implement QI activities in the facility. The team identified a quality gap as the facility was not screening mothers for anaemia during antenatal care clinics. Instead, the mothers were referred to the nearest facility located 20km away (Turbo Sub County hospital) where the test could be done. Anaemia in pregnancy is not only a key topic covered during integrated ANC & PNC training by LSTM; but also, a major risk factor because pregnant mothers with anaemia face a higher risk of bleeding after delivery. In Kenya, obstetric haemorrhage is the number one cause of maternal mortality accounting for 2 out of every 5 maternal deaths (CEMD report 2017).
The baseline measurement for Quality MNH Standard 1.2.4 “All women attending for ANC are screened for anaemia and treated if found positive.” was 36% of women attending ANC at Ngenyilel health centre screened for anaemia. This was because not all the ANC patients could afford the transport to travel 20km to obtain the test at the sub-county hospital. The QIT proposed to the facility management to procure a HaemoCue testing machine however, the facility lacked the necessary resources neither did the county. The QIT explored the options of collecting the blood samples and sending them to Turbo hospital for testing. In liaison with Jessica Mwalema, Subcounty Reproductive Health (RH) coordinator, Turbo hospital agreed to receive the blood samples from Ngenyilel staff and conduct Hb testing. The test results are collected, recorded in the ANC register, and mothers found to have anaemia receive appropriate treatment at the health centre on the subsequent ANC visit. After a couple of months, the subsequent evaluation showed that 88% of women attending ANC at Ngenyilel health center had been screened for anaemia, and those who were positive received treatment.
Before the training by LSTM, we didn’t know about Quality Improvement. But now we know and feel good because we are serving clients with the right information, and providing quality care during pregnancy, childbirth, and postnatal period”.
Ben Too, Nurse at Ngenyilel Health centre
In May 2023, while conducting a support-supervisory visit to Ngenyilel Health centre, subcounty RH coordinator (Jessica) confirmed above-mentioned statistics and witnessed the procedure in practice.

The facility manager, Janet Chepkemoi affirmed that under Kenya’s ‘Linda Mama’ health scheme for pregnant mothers, services at the facility are offered free of charge; however the blood testing equipment at the facility laboratory is not functional. Quality Champions in all supported facilities working with QITs, are finding pragmatic solutions to quality improvement challenges, supported by the LSTM Kenya technical team.
I volunteer to carry the blood samples to and from Turbo SCH for testing; And so, do all other staff who may be enroute to Turbo at some point. Because when we refer the mothers to go by themselves for the blood test at Turbo SCH, they face a challenge with meeting transport costs and eventually only a few make it”.
Janet Chepkemoi, Facility Manager at Ngenyilel Health“Without quality, universal health coverage remains an empty promise. Even with increased access to services, health improvements can remain elusive unless those services are of sufficient quality to be effective.” Dr Tedros Adhanom Ghebreyesus (WHO Director-General @Global Ministerial Summit – Jeddah)
With support from Takeda CSR program, and through Global Fund, LSTM remains committed to improving the quality of integrated ANC and PNC, working in collaboration with National MoH and county health departments of Uasin Gishu, Vihiga and Garissa.