Researchers led by LSTM’s Dr. Gabriela Gomes have demonstrated, in a paper published today in the journal Nature Communications, how to measure differences amongst individuals in relation to the acquisition of tuberculosis (TB) to improve predictions made by mathematical models.
Dr. Gomes said: “Global stakeholders including the World Health Organization rely on predictive models for developing strategies and setting targets to control or eliminate infectious diseases. However, as model-informed policies are being implemented, the inaccuracy of some predictions becomes apparent, at times substantially overestimating the impact of interventions over time. Our paper examines this issue with reference to the targets set for tuberculosis elimination.”
The paper explains how limitations in capturing the effects of heterogeneity present in real-world settings could play a major role in the observed discrepancies. Individual variation in risk of infection and disease is due to many factors, including age, habits, general health status, home environment, social connections, and more. To reconstruct the risk of each individual by measuring an open-ended list of variables and their interactions is impossible. To advance amidst such difficulties and contribute constructively to the development of health policies, the paper proposes the adoption of new metrics – risk inequality coefficients (RIC) – that capture inequality without specifying the underlying factors.
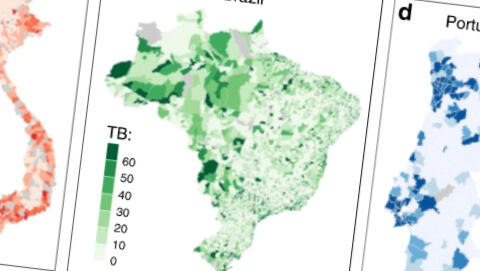
Looking at the countries of Brazil, Portugal, and Vietnam, Dr. Gomes Explained: “Applying this approach to 14 years of tuberculosis incidence data we identified the acquisition of infection as the single process where heterogeneity most fundamentally impacts model outputs. Our results imply that in Portugal and Vietnam consistent declines in TB incidence was a result of reducing progression to disease from recent infection, while similar declines in TB in Brazil might be related to reductions in the rates of reactivation from latent TB. Importantly, this difference leaves Brazil with more optimistic prognostics for meeting the incidence targets set by the WHO End-TB strategy post-2015.”
The work was conducted under the auspices of the World Health Organization and the French Institute for Research in Sustainable Development (IRD, Montpellier, France). For Dr Christian Lienhardt, from IRD: “the adoption of risk inequality metrics such as the RIC will enable policymakers to assess risk inequality in each country, compare the metric across countries, and monitor the impact of equalization strategies and targeted interventions over time.”
M. Gabriela M. Gomes, Juliane F. Oliveira, Adelmo Bertolde, Diepreye Ayabina, Tuan Anh Nguyen, Ethel L. Maciel, Raquel Duarte, Binh Hoa Nguyen, Priya B. Shete & Christian Lienhardt
Introducing risk inequality metrics in tuberculosis policy development
Nature Communications 10, Article number: 2480 (2019) 2019/06/06
doi.org/10.1038/s41467-019-10447-y