LSTM’s seminar series continued yesterday with a presentation by Dr Catherine O’Neill, senior lecturer within the Dermatology group of the University of Manchester’s Institute of Inflammation and Repair. Her seminar, “Topical probiotics – new approaches to the maintenance and repair of the skin barrier”, was introduced by LSTM’s Dr Alvaro Acosta-Serrano.
Dr O’Neill started by explaining exactly what probiotics were, using the WHO definition of “live microorganisms which when administered in adequate amounts confer a health benefit on the host”. These microorganisms are mainly derived in the gut and are seen as generally safer and conferring a health benefit. Dr O’Neill’s team sought to establish if they worked on other kinds of tissue other than the gut, and do they need to be ingested, or can they be used topically.
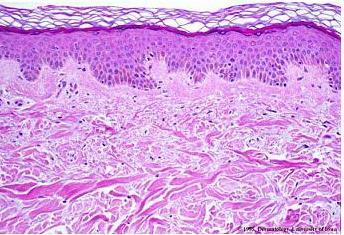
She went on to explain the structure of the human skin, with its three layers, looking most closely at the epidermis, the outer layer of skin which is constantly renewing itself, shedding of millions of skin cells per cm2 every day. She then looked at the microbiota living on the skin, explaining the different kind bacteria that live on the different kinds of skin area, emphasising that anatomical location is key in terms of bacteria that lives there.
She then posed the interesting question about what the skin microbiota does. While there is no strong evidence that it can prevent colonisation of pathogens, it is known to able to trigger the release of antimicrobial peptides (part of the innate response) from keratinocytes (main epidermal cells) and so it seems to enhance the immune system. However, it can also be pathogenic itself if specific bacterial populations increase.
It has previously been assumed that the epidermis acted as a barrier, but recent work, highlighting the fact that DNA from bacteria has been found in at deeper levels, poses the question “does it in fact act as a filter?” If it acts as a filter, it would explain why bacteria can inflame the flare up in some skin conditions which has lead Dr O’Neill’s team to look at whether reprofiling of the skin microbiota would be useful therapy.
While reprofiling using skin commensals would pose difficulties due to the anatomical site differences in microbiota, combined with massive interpersonal variation, her team looked instead at three issues using gut commensals. First they looked at what would happen if they added different gut probiotics topically to the skin to protect it from the bacteria Staphylococcus aureus. The probiotics acted differently, protecting the keratinocytes if added before or at the same time as the S. aureus. It is supposed that this is partly because it stops S. aureus from binding with the skin, which is backed up by the fact that the probiotic that didn’t work did not bind with the keratinocytes.
Dr O’Neill’s group went one step further to see if the damage could be repaired by adding L. rhamnosus GG 12 hours after incubation with pathogenic bacteria. They found that it was still able to rescue the keratinocytes not only by blocking the adhesion but also by limited the growth of S. aureus.
She then explained how the team looked at the role of probiotic bacteria lysates in barrier repair, finding that scratches healed much quicker when lysates from L. rhamnosus GG was applied topically. This was further tested by using biopsied human skin, which was put into nutrient poor environments. When L. rhamnosus GG lysate was added it promoted the skins re-epithelial growth.
They also looked at the effects of the lysates of prebiotic bacteria on the function of tight junctions, which sit between the epithelial cells protecting from pathogens in the first living layers of skin. They found that the addition of such lysates increased tight junction protein expression in human skin.
She concluded by talking about the further research that should be undertaken, but also looked at the great potential for use on the skin and its possible applications, ranging from wound repair, to barrier strengthening and cosmetic s preparation.
